Squamous Cell Carcinoma Treatment
Introduction
Cutaneous squamous cell carcinoma (SCC) is the second most common form of skin cancer and accounts for 20% of cutaneous malignancies.1 Squamous cell carcinoma frequently arises on the sun-exposed skin of middle-aged and elderly individuals. Most squamous cell carcinomas are readily identified and removed in the physician's office as a minor surgical procedure. Larger and more invasive lesions may require aggressive surgical management, radiation therapy, or both. High-risk squamous cell carcinoma carries a significant risk of metastasis and, as such, requires careful evaluation and treatment.
General risk factors associated with the development of squamous cell carcinoma are as follows
- Age older than 50 years
- Male sex
- Light skin; blonde or light brown hair; green, blue, or gray eyes
- Skin that sunburns easily (Fitzpatrick skin types I and II)
- Geography (closer to the equator)
- History of prior nonmelanoma skin cancer
- Exposure to UV light (high cumulative dose of sunshine, tanning beds, or medical UV treatments)
- Exposure to chemical carcinogens (eg, arsenic, tar)
- Exposure to ionizing radiation (medical treatments, occupational or accidental radiation exposure)
- Chronic immunosuppression
- Chronic scarring conditions
- Certain genodermatoses
- Human papillomavirus (HPV) infection (specific subtypes)
Pathophysiology
Squamous cell carcinoma is a malignant tumor of epidermal keratinocytes. Some cases of squamous cell carcinoma occur de novo (ie, in the absence of a precursor lesion); however, some squamous cell carcinomas arise from sun-induced precancerous lesions known as actinic keratoses (AKs). Patients with multiple AKs are at increased risk for developingSquamous cell carcinoma is capable of locally infiltrative growth, spread to regional lymph nodes, and distant metastasis, most often to the lungs.
Frequency United States
Determining the true incidence of squamous cell carcinoma is difficult because health registries exclude nonmelanoma skin cancer (including squamous cell carcinoma) from their databases because of the high number of cases and limited resources to collect data and because the rate of squamous cell carcinoma varies based on geographic locale. In 1994, the annual incidence in the United States ranged from 81-136 cases per 100,000 population for men and 26-59 cases per 100,000 population for women. Studies also confirm a dramatic increase in the incidence of cutaneous squamous cell carcinoma over the past several decades. For example, in Rochester, Minnesota, the annual age-adjusted incidence rates of squamous cell carcinoma per 100,000 women rose from 47 cases from 1984-1986 to 100 cases from 1990-1992. The corresponding rates for men increased from 126 cases to 191 cases per 100,000 population
One reason for the rising incidence of squamous cell carcinoma may be an increase in sun exposure in the general population. Some postulate that ozone depletion may be intensifying UV exposure. Other factors that may contribute to the increased incidence of squamous cell carcinoma include the advancing age of the US population, earlier and more frequent diagnosis of squamous cell carcinoma due to enhanced public awareness of skin cancer, and more frequent skin examinations by physicians.
Additionally, the number of patients on immunosuppressive therapy, used in solid organ transplantation and various rheumatologic and dermatologic conditions, is increasing. Squamous cell carcinoma formation has been associated with immunosuppressive drug therapy in solid organ transplantation patients, who have a markedly elevated risk of squamous cell carcinoma formation. Metastasis also may be more common in this group.
International
Prevalence rates of squamous cell carcinoma vary in different countries. The highest incidence occurs in Australia, where the age-adjusted incidence has been calculated to be 1332 cases per 100,000 population for men and 755 cases per 100,000 population for women. Again, this is likely due to large numbers of light-skinned people in this region who have had extensive sun exposure
Mortality/Morbidity
Most squamous cell carcinomas are readily treated and produce few sequelae. A subset of high-risk lesions causes most of the morbidity and the mortality associated with squamous cell carcinoma. Such lesions may cause extensive destruction of tissue, and their removal may entail substantial cosmetic deformity. The overall risk of metastasis for squamous cell carcinoma is in the range of 2-6%; however, rates as high as 47% have been reported for cases with extensive perineural invasion. Lymph node metastasis is associated with significant morbidity; however, 5-year survival rates as high as 73% have been achieved with the combination of surgical lymphadenectomy and radiation therapy.Once lung metastasis occurs, the disease is currently incurable.
Race
Squamous cell carcinoma is the second leading cause of skin cancer in whites.Persons of Irish or Scottish ancestry have the highest prevalence in the United States. Squamous cell carcinoma is relatively rare in people of African and Asian descent, although it is the most common form of skin cancer in these groups. Squamous cell carcinoma in blacks carries a higher mortality rate, perhaps due to delayed diagnosis because tumors are more likely to occur in sun-protected areas, including the scalp and sites of previous injury and scarring
Sex
Squamous cell carcinoma occurs in men 2-3 times more frequently than it does in women, most likely as a result of greater cumulative lifetime UV exposure.
Age
The typical age at presentation is approximately 70 years; however, this varies widely, and, in certain high-risk groups (eg, organ transplant recipients [OTRs], patients with epidermolysis bullosa), squamous cell carcinoma often manifests at a much younger age.
Clinical History
A detailed patient history often reveals the presence of one or more risk factors for squamous cell carcinoma (SCC) (see general risk factors in Background). Most squamous cell carcinomas are discovered by patients and are brought to a physician's attention by the patient or a relative. The typical squamous cell carcinoma manifests as a new or enlarging lesion that concerns the patient. Squamous cell carcinoma is typically a slow-growing malignancy, but some lesions enlarge rapidly. Although most squamous cell carcinoma patients are asymptomatic, symptoms such as bleeding, weeping, pain, or tenderness may be noted, especially with larger tumors. Numbness, tingling, or muscle weakness may reflect underlying perineural involvement, and this history finding is important to elicit because it adversely impacts prognosis
- Actinically derived squamous cell carcinoma: The most common type of squamous cell carcinoma is the sun-induced type. As such, a history of long-term sun exposure dating back to childhood is frequently elicited. Many patients report having experienced multiple blistering sunburns during their lifetime, while others may have used indoor tanning beds or received UV light therapy (eg, psoralen plus UVA [PUVA] for psoriasis). Patients may have been treated in the past for sun-induced lesions such as AKs, basal cell carcinoma (BCC), melanoma, or squamous cell carcinoma.
- Immune suppression: Patients should always be questioned about possible sources of immunosuppression. A history of solid-organ transplantation, hematologic malignancy (particularly chronic lymphocytic leukemia [CLL]), HIV infection or AIDS, or long-term use of immunosuppressive medications (eg, as treatment for an autoimmune condition) may be elicited.
- Marjolin ulcer: This eponym refers to a squamous cell carcinoma that arises from chronically scarred or inflamed skin. Patients may report a change in the skin (eg, induration, elevation, ulceration, weeping) at the site of a preexisting scar or ulcer. The latency period is often 20-30 years; therefore, the diagnosis requires a high index of clinical suspicion.
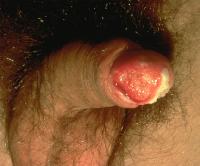
- HPV-associated squamous cell carcinoma: Virally induced squamous cell carcinoma most commonly manifests as a new or enlarging warty growth on the penis, vulva, perianal area, or periungual region. Patients often present with a history of "warts" that have been refractory to various treatment modalities in the past. A history of previously documented genital HPV infection may be elicited.
Physical
Squamous cell carcinoma (SCC) may manifest as a variety of primary morphologies with or without associated symptoms.
- Squamous cell carcinoma in situ (SCCis): Squamous cell carcinoma in situ is defined histologically by atypia involving the full thickness of the epidermis but without invasion into the dermis. Clinically, lesions of squamous cell carcinoma in situ range from a scaly pink patch to a thin keratotic papule or plaque similar to an AK. Bowen disease is a subtype of squamous cell carcinoma in situ characterized by a sharply demarcated pink plaque arising on non–sun-exposed skin. Erythroplasia of Queyrat refers to Bowen disease of the glans penis, which manifests as one or more velvety red plaques.
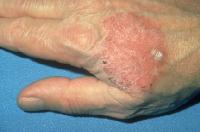
Squamous cell carcinoma in situ, Bowen disease. Courtesy of Hon Pak, MD.
 Typical squamous cell carcinoma: The characteristic invasive squamous cell carcinoma is a raised, firm, pink-to-flesh–colored keratotic papule or plaque arising on sun-exposed skin. Approximately 70% of all squamous cell carcinomas occur on the head and neck, with an additional 15% found on the upper extremities. Surface changes may include scaling, ulceration, crusting, or the presence of a cutaneous horn. Less commonly, squamous cell carcinoma may manifest as a pink cutaneous nodule without overlying surface changes. The absence of surface changes should raise suspicion of a metastatic focus from another skin or nonskin primary site or a different and potentially more lethal tumor such as Merkel cell carcinoma. A background of severely sun-damaged skin, including solar elastosis, mottled dyspigmentation, telangiectasia, and multiple AKs, is often noted.
Typical squamous cell carcinoma: The characteristic invasive squamous cell carcinoma is a raised, firm, pink-to-flesh–colored keratotic papule or plaque arising on sun-exposed skin. Approximately 70% of all squamous cell carcinomas occur on the head and neck, with an additional 15% found on the upper extremities. Surface changes may include scaling, ulceration, crusting, or the presence of a cutaneous horn. Less commonly, squamous cell carcinoma may manifest as a pink cutaneous nodule without overlying surface changes. The absence of surface changes should raise suspicion of a metastatic focus from another skin or nonskin primary site or a different and potentially more lethal tumor such as Merkel cell carcinoma. A background of severely sun-damaged skin, including solar elastosis, mottled dyspigmentation, telangiectasia, and multiple AKs, is often noted.
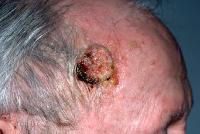
Large sun-induced squamous cell carcinoma on the forehead/temple.
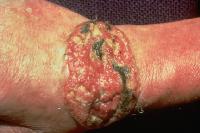
Squamous cell carcinoma. Courtesy of Hon Pak, MD.
Periungual squamous cell carcinoma: Periungual squamous cell carcinoma typically mimics a verruca and is frequently misdiagnosed for years as a wart prior to biopsy. Less commonly, lesions may resemble chronic paronychia with swelling, erythema, and tenderness of the nail fold; onychodystrophy also may be noted.
- Marjolin ulcer: This subtype of squamous cell carcinoma appears as a new area of induration, elevation, or ulceration at the site of a preexisting scar or ulcer. Patients with this form of squamous cell carcinoma can have a poor prognosis. The diagnosis of Marjolin ulcer should be considered in any ulcer that fails to heal with standard therapy.
- Perioral squamous cell carcinoma: Squamous cell carcinoma of the lip usually arises on the vermillion border of the lower lip. It is sometimes predated by a precursor lesion, actinic cheilitis, which manifests as xerosis, fissuring, atrophy, and dyspigmentation. Actinic cheilitis is analogous to AK of the skin. Squamous cell carcinoma on the lip manifests as a new papule, erosion, or focus of erythema/induration. Intraoral squamous cell carcinoma typically manifests as a white plaque (leukoplakia) with or without reddish reticulation (erythroplakia). Common locations include the anterior floor of the mouth, the lateral tongue, and the buccal vestibule.
- Anogenital squamous cell carcinoma: Squamous cell carcinoma in the anogenital region may manifest as a moist, red plaque on the glans penis; indurated or ulcerated lesions may be seen on the vulva, external anus, or scrotum. Associated symptoms include pain, pruritus, and intermittent bleeding.
- Verrucous carcinoma: Verrucous carcinoma is a subtype of squamous cell carcinoma that can be locally destructive but rarely metastasizes. Lesions appear as exophytic, fungating, verrucous nodules or plaques, which may be described as "cauliflowerlike." Verrucous carcinoma is further subdivided based on its location in the anogenital region (Buschke-Löwenstein tumor), the oral cavity (oral florid papillomatosis), and the plantar foot (epithelioma cuniculatum).
- Lymphadenopathy: With any invasive (not in situ) squamous cell carcinoma, regional lymph nodes should be examined. Lymph node enlargement must be further evaluated by fine-needle aspiration (FNA) or nodal biopsy.
Causes
The primary cause of most squamous cell carcinoma (SCC) is cumulative lifetime sun exposure. The frequency of squamous cell carcinoma is increased at lower latitudes, correlating with an increased intensity of ambient light. Other causes of squamous cell carcinoma are discussed below.
- UV sunlight exposure
- The component of sunlight believed to be most important in cutaneous carcinogenesis is UVB (290-320 nm), which is both an initiator and a promoter of carcinogenesis. In animal models, UV-induced photocarcinogenesis appears to involve the UVB and UVA-2 spectral ranges
- UVB-induced photocarcinogenesis appears to work by suppressing the immune system in several ways. The UVB spectrum inhibits antigen presentation, induces the release of immunosuppressive cytokines, and elicits DNA damage, specifically the generation of pyrimidine dimers in keratinocyte DNA that is a molecular trigger of UV-mediated immunosuppression
- Inactivation of the tumor suppressor gene TP53 occurs in up to 90% of all cutaneous squamous cell carcinoma lesionsOther tumor suppressor genes found to be mutated in squamous cell carcinoma include P16 (INK4a) and P14 (ARF)
- Therapeutic UV exposure: UV light treatments used for psoriasis (and other recalcitrant dermatoses) also predispose to the development of squamous cell carcinoma. PUVA is particularly phototoxic and mutations in both TP53 and the oncogene Ha-Ras are present in a large proportion of PUVA-associatedIn addition to being mutagenic, UVA in conjunction with UVB is a potent suppressor of the cutaneous immune system, which likely contributes to its role in cutaneous carcinogenesis.
- Fair complexion: Individuals with skin types I and II account for most of the patients who develop squamous cell carcinoma; patients with oculocutaneous albinism are also at risk, and squamous cell carcinomas account for the most common type of cutaneous malignancy in this group. Such individuals lack natural protection from UV-induced carcinogenesis, owing to reduced levels of the photoprotective pigment, melanin
- Ionizing radiation: Therapeutic ionizing radiation is typically associated with the later development of BCCs, but the risk of developing squamous cell carcinomas is also increased Most patients with radiation-induced tumors have a remote history of x-ray therapy for acne vulgaris, although patients developing squamous cell carcinoma in radiation ports for Hodgkin disease or thyroid cancer treatment is not uncommon.
- Chemical carcinogens: Exposure to arsenic is a well-established cause of cutaneous squamous cell carcinoma and internal cancers.Today, the main source of arsenic is contaminated well water, although arsenic may also be found in traditional Chinese medicines. Other carcinogens associated with squamous cell carcinoma include polycyclic aromatic hydrocarbons such as tar, soot, and pitch.
- DNA repair failure: Healthy human skin is constantly repairing UV-induced damage through DNA repair mechanisms. Patients with xeroderma pigmentosum have a deficiency in an enzyme essential for normal DNA repair and are thus prone to the development of innumerable squamous cell carcinomas, and, less commonly, other cutaneous tumors
- Iatrogenic immunosuppression: The use of immunosuppressive medications to prevent rejection in OTRs is associated with a 65- to 250-fold increased risk of developing squamous cell carcinoma compared with the general population
- The primary risk factor in these patients is cumulative lifetime UV exposure in combination with having skin type I or II. This risk also increases with the number of years posttransplantation, presumably because of the cumulative effects of prolonged immunosuppressive therapy.
- The greatest risk occurs in heart transplant patients, with diminishing risk seen in recipients of kidney and liver transplants, which correlates with the degree of immunosuppression (ie, number and/or dosage of medications) typically required to prevent rejection in these patient populations.
- Pretransplantation end-organ disease may also impact the development of posttransplant squamous cell carcinoma. For example, among renal transplant recipients, the highest prevalence of skin cancer was observed in patients with polycystic kidney disease, while the lowest incidence was seen in those with diabetic nephropathy. Similarly, cholestatic liver disease was associated with a greater posttransplantation risk of skin cancer compared with other causes of liver failure.
- Noniatrogenic immunosuppression: In addition to iatrogenic immunosuppression, defects in cell-mediated immunity related to lymphoproliferative disorders (eg, CLL) predispose to the development of aggressive squamous cell carcinoma. The specific mechanisms by which immunosuppression leads to squamous cell carcinoma development are poorly understood, but diminished immunosurveillance is thought to be critical. CD8+ T cells specific for the tumor suppressor gene TP53 have been observed in patients with squamous cell carcinoma, suggesting that a functional immune system may target keratinocytes expressing mutated TP53 Suppression of the immune system would presumably abrogate this response and might be expected to facilitate the development of squamous cell carcinoma.
- HPV: Infection with specific subtypes of HPV is believed to play a role in the development of anogenital and periungual squamous cell carcinoma. HPV types 6 and 11 are associated with Buschke-Löwenstein tumors, whereas HPV type 16 has been frequently identified in both genital and periungual squamous cell carcinoma, suggesting the possibility of genital-digital spreadHPV types 5 and 8 are associated with cutaneous squamous cell carcinoma in transplantation patients
- Chronic inflammation
- Chronic inflammation, irrespective of the underlying etiology, may lead to the development of squamous cell carcinoma. Both noninfectious inflammatory diseases and chronic infections have been associated with squamous cell carcinoma.
- Likewise, the Marjolin ulcer variant of squamous cell carcinoma may develop in patients with a chronic scarring condition such as dystrophic epidermolysis bullosa. In fact, the leading cause of death in patients with dystrophic epidermolysis bullosa is metastatic cutaneous squamous cell carcinoma.More recently, evidence suggests that patients with junctional epidermolysis bullosa may also be at increased risk for developing The underlying pathogenesis of such lesions is not understood, but mutations in the TP53 and P16 tumor suppressor genes have been described in dystrophic epidermolysis bullosa–associated
- Some of the conditions that predispose to the development of squamous cell carcinoma are highlighted as follows: